Villanova Nursing Graduate Students on the Frontline

Stacey Ambrose, BSN, RN- BC, CHPN
Adult-Gerontology Nurse Practitioner Student, Fitzpatrick College of Nursing
Telemetry nurse, Paoli Hospital, Main Line Health, Paoli, PA
June 21, 2020
As a nurse, you never know what you are walking into when you come to work. When I came into to work in late March, I found that I was getting pulled to the Progressive Care Unit (PCU). COVID-19 was just starting to be community spread, and I really wasn’t sure what I would be walking into. Arriving to the PCU, I had two groups to choose from: COVID or non-COVID. I chose the COVID group. I had recently recovered from the virus and felt that I should help reduce exposure to any other nurse. I had no idea how that choice would impact my life.
I only had one patient, a woman in her late 80s who had likely contracted COVID at her husband’s funeral a few weeks earlier. I got report from the previous shift and went in to meet my patient. She could just barely find the energy to speak over the force of the air from the BiPap machine that was helping her breathe. Though she worked so hard to breathe, she remained attentive and cooperative to the questions of my assessment, but within our first interaction she let me know she felt her body shutting down. She also wanted to make sure she spoke to her daughter, and with that I thought my goal for the shift was developed. Speaking to her daughter was what meant the most to her this day, and that is what my nursing care would deliver.
The next time I was in the room, I transitioned her from the BiPap to a non-rebreather mask to ensure good oxygenation and helped her make the call. Unfortunately, she was only able to talk to her daughter for a few minutes before she needed the support of the BiPap again. I placed her back on the BiPap made sure she was comfortable and left her room.
When I came back to check on her the next time, she made it even more clear that she felt her body shutting down. She recounted her memories of watching her husband and parents succumb to illness and knew that her body was doing the same. I tried to reassure her that this could pass, but she was insistent that she wanted to let her body shut down. I knew I had to do something.
I reached out to our Palliative Care nurse, who had worked with the patient and daughter the day before, to let her know that the patient was requesting for all of the machines to be stopped. She made phone calls to the daughter and immediately began making arrangements to honor this woman’s wishes.
I have walked into work so many times, and so many different scenarios have been placed in front of me, but never one like this. A patient dying from a virus we know nothing about, and no family allowed to be there to support her. I knew the first thing that I needed to do was to reach out to the daughter. Although she was overjoyed to talk to her daughter earlier, she was hesitant to speak to her now. Sadly, she thought that we wanted to ask her daughter for permission, but I explained that her daughter needed to hear her voice one more time. Fortunately, we made that call because afterward she was also able to speak to her granddaughter. I worked as a translator through the BiPap and will never forget the look on her face when I repeated her granddaughter words, “You are the greatest influence I have ever had, I love you so much!” A look of humility that showed the humble manner in which this woman carried herself overtook her as I repeated those words to her.
The Palliative Care nurse and our hospice nurse came to the floor and helped to develop a plan to make her comfortable with medication. After I had everything in place, I entered the room and explained the plan to the patient to which she assented. In our last exchange, I thanked her for being my patient and reminded her how lovely it was to be at her side. Shortly after I injected the medicine she fell into a deep sleep and her body became comfortable and breathing eased. After a little wait we were able to remove the BiPap while she remained comfortably sleeping until her last breath in the middle of the night.
Never before has a case so deeply affected me. I was blessed to be by the side of someone who so clearly was able to make her wishes known and honored to be the substitute for the comforting hands of her family. As nurses we never know what we will walk into when we come to work, but we should always know there is an opportunity to make a profound difference in someone’s life.

Ana Silva, BSN, RN-BC
Adult-Gerontology Nurse Practitioner Student, Fitzpatrick College of Nursing
Medical-Surgical pool nurse; Thomas Jefferson University Hospital, Philadelphia
March 31, 2020
I have been working at the drive up/walk up COVID-19 testing site outside of my hospital for a few weeks.
Honestly, until this pandemic my use of an N95 mask was limited to a handful occasions lasting thirty minutes to an hour maximum. I could just use it and throw it away with the rest of my PPE after that patient interaction where it was needed. Fast forward to now, wearing the same N95 for hours in addition to an isolation gown, gloves and goggles outside, feels surreal.
I will say that I am proud to be in a position to help during this public health crisis. There is a small fear that I am risking exposing my husband and four kids when I come home from testing these patients, but I remind myself that I am as protected as I can be. For now, I am supplied with all the PPE I need for this circumstance.
Although my working environment can be uncomfortable at times because of the weather and continuous mask wearing, I am proud to do it.

Vanessa Peffall, RN, BSN
Family Nurse Practitioner Student, Fitzpatrick College of Nursing
eICU RN, PENN Medicine, Philadelphia
March 29, 2020
I am monitoring my assignment of patients in the ICUs at Penn Medicine.
I am proud to be a nurse. I am grateful for the opportunity to be able to assist my colleagues who are on the front lines.
Villanova is an extremely supportive and encouraging environment that gives me the confidence to know that we are truly making a difference during such uncertain and challenging times.
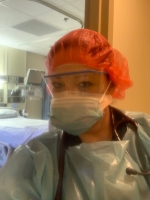
Theresa Dobbin, BSN, RN, CCRN, WCC
Adult-Gerontology Nurse Practitioner Student, Fitzpatrick College of Nursing
Staff RN, Critical Care Unit (CCU)
RWJ Barnabas Rahway, Rahway, NJ
March 28, 2020
In this photo, I just put on all of my personal protective equipment (PPE) to prepare for another COVID-19 patient who was being admitted to our unit. I'm thankful we have an empty bed behind me in the one photo to be able to care for the patient that needs us at this time.
I've been an RN for 30 years after graduating from Wagner College in 1990, and I have never been in a situation like this before. While I'm at work, we take care of our patients like we have always been doing, but under more stressful conditions.
We don’t know what the next several weeks or months will bring, so we are going to prepare the best that we can. I feel hopeful that this too shall pass, but also nervous about having the equipment and supplies to properly care for these patients.
I have never been more proud to be nurse. The teamwork in our unit and beyond our unit is amazing. We have truly come together as an interdisciplinary team to care for our patients. The outside community providing food for us, sending handmade cards and sewing masks for us has been overwhelming.
The Nurse Practitioner Program at Villanova University has helped me to become a better nurse. My assessment skills have improved over the past several months, and what better time to utilize my skills than during a global pandemic.
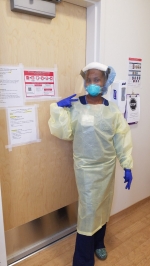
Hellen Nyamu, BSN, RN
Family Nurse Practitioner student, Fitzpatrick College of Nursing
Emergency Room, John's Hopkins Hospital, Baltimore, MD
March 28, 2020
The FNP program at Villanova has been pivotal in my preparedness of handling difficulty, and stressful situations. However, I did not anticipate a rather quick test to my professional agility and resilience.
COVID-19 has affected each one of us personally, and really changed how we do health care. Yet, it has drawn our strengths in working together as a team with a clear focus.
Here at Johns Hopkins, we are at the front lines of the battle with COVID-19 as it with so many other health care workers all over the world. We have learned how to quickly improvise and use scarce resources wisely. I have seen great team efforts in making things happen quickly, and efficiently.
It has been a great honor to feel needed and to save a life.